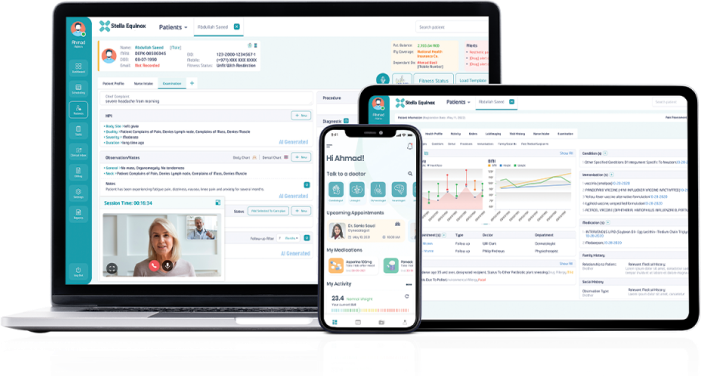
Equity is a current buzzword for many, but for us, it has been our lifeblood and motivation
from Stella's beginnings. Stella Equinox is a cloud-based EMR specifically built to overcome
barriers to care for underserved patients in remote areas. Our early managers traveled
throughout the deserts and mountains of Pakistan setting up remote clinics to pilot
telemedicine programs there. As Hussnain Khursheed, the Director of Business Development and
Sales at Stella, says, "Stella Equinox covers a part of society that has been ignored, which
does not have access to basic healthcare services."
Stella hopes to bring Equinox to many more people who need it throughout
the world. Our Equinox clients include clinics in the United Arab Emirates (UAE), which are
integrated with Health Information Exchanges (HIEs) Malaffi (the first HIE in the Middle
East), Riayati and Nabidh. Currently, we are working on bringing Equinox to emerging markets
in the Middle East, Africa, and Asia. That's because we believe that everyone deserves equal
access to quality healthcare.






























.d1fafe55.png)